Need Help?
We are here to help.
We care for each one who come to us with hope in their hearts.

AMH (Anti-Mullerian Hormone) is a glycoprotein hormone secreted by pre-antral follicles and small antral follicles of the ovary. Low AMH is the result of a malfunction in its secretion for multiple reasons that we’ll discuss in the next section.
When required, an AMH test measures the levels of anti-mullerian hormone in the body, with the resultant levels representative of a woman’s egg count. For example, low AMH can indicate reduced egg count, and high AMH represents higher egg counts. The hormone can also help determine if the baby has functioning testicular tissue.
By puberty, a woman has about 100,000 eggs in the ovaries. When she reaches around 40 years of age, fewer than 10,000 eggs remain. Naturally, the result of that is low levels of AMH. Menopause is reached when no eggs are left in the ovaries, and the reproductive organs do not have to prepare themselves every month for pregnancy.
If a woman presents with drastically low levels of AMH before the age of around 40, it indicates a reproductive issue.
AMH tests reveal the potential of a woman to get pregnant. The test can be conducted on any day of the menstrual cycle. The other tests of ovarian reserve, such as the Follicle-Stimulating Hormone (FSH) test, must be performed on a specific day of the period. For example, day 1 or day 2 of the menstrual cycle.
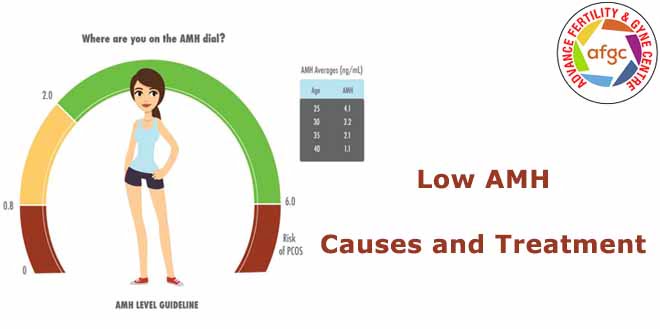
The normal range for AMH levels is between 1 and 3.5 ng/ml. Any AMH level above 2 ng/ml is considered a good value, and a level <1 ng/ml is considered low. Levels below 0.3 ng/ml are considered very low.
Women with polycystic ovaries have AMH levels > 3.5 ng/ml. AMH level reduces with age; younger women usually have AMH > 3.5 ng/l, and women over 40 years old have < 1 ng/ml.
AMH can also be expressed as picomol/ml, where the values multiply by a factor of 7.
There are several causes of low levels of AMH. Some of the most common include:
Age
Genetic factor
Autoimmune diseases
Cancer treatment
Excessive smoking
Environmental issues
Obesity
The Symptoms of low AMH vary from woman to woman. Some of the most common symptoms of low AMH include:
Irregular menstruation
Difficulty conceiving naturally
Low libido
Fatigue
Hot flashes
Elevated FSH levels
Early menopause
Typically, there are no specific low AMH treatment options available. However, with adequate lifestyle management, taking vitamins and supplements can improve pregnancy outcomes significantly.
Low AMH treatment is more about how women treat their bodies to slow the reduction of egg count. That being said, there are some treatment options available that we’ll discuss in the next section.
Despite treatment options being limited and centred around lifestyle changes, at Advance Fertility and Gynae Centre, we have had reasonable success treating women with low AMH. One must know that having low levels of AMH does not mean you cannot get pregnant. Older women with reduced AMH levels fare much worse than younger women.
Multiple cycles of stimulation may result in improved egg numbers in subsequent cycles. Antagonists and long protocols work equally well. We’ve also noticed that embryo pooling is helpful. Additionally, early cleavage transfer is better than blastocyst, and routine PGS is not recommended.
We understand that going through repeated cycles to get your hormones and lifestyle fixed can be daunting for some. We understand the challenge of many women who have finally decided to embrace motherhood. At Advance Fertility Clinic, we are compassionate and driven to help you take steps towards becoming a mother.
Our state-of-the-art labs are equipped to conduct a wide range of tests to determine your current health conditions. Based on these real-time test results, we recommend methods that make it possible for you to conceive. Our goal is to help you reach your dream of becoming a parent.
Reduce excessive exposure to sunlight.
Consume more green leafy vegetables.
Avoid packaged foods that are high in preservatives.
Incorporate more fiber into your diet.
Eat small but nutrient-rich meals to support your bodily functions.
Reduce exposure to factors that cause stress.
If you can’t balance your AMH levels naturally, our expert team may recommend supplements and vitamins that can support the production of AMH in the body.
We also offer a wide range of infertility treatments and IVF processes that have a higher success rate.
If you are considering getting pregnant, contact our experts by calling +91-9871250235 or by emailing contact@advancefertility.in today. We’re ready to help you find the infertility treatment plan that is exclusive to your specific health condition and needs.
The causes of low AMH (Anti-Mullerian Hormone) levels can include advanced age, diminished ovarian reserve, certain medical conditions, and genetic factors. Reduced ovarian egg production can affect fertility, and low AMH is frequently a sign of this.
At Advance Fertility, ovarian reserve testing, hormonal assessments, blood tests, and comprehensive fertility assessments are used to diagnose the underlying causes of low AMH. Our specialists are able to pinpoint the precise causes of low AMH levels thanks to this in-depth investigation.
While age is a predominant factor, certain lifestyle factors like smoking and excessive stress may contribute to low AMH levels. At Advance Fertility, we take a holistic approach to treating patients with low AMH, taking into account lifestyle factors.
Early detection of low AMH is significant as it allows for proactive fertility management. Early detection of low AMH levels allows for prompt treatment planning and intervention, increasing the likelihood of successful reproductive outcomes.
While low AMH can pose challenges, it does not eliminate the possibility of successful fertility treatments. Our skilled team at Advance Fertility uses cutting-edge methods and customized strategies to maximize results, even in situations with low AMH, giving people who want to start a family hope.
We care for each one who come to us with hope in their hearts.

Disclaimer – Dr Kaberi is not associated with any Hosptial/Clinic other than “Advanced Fertility and Gyne Center (AFGC)”. AFGC has only four centers at present 1. “Lajpat Nagar” 2. “CR Park Delhi” 3. “Noida” 4. “Gurgaon“.